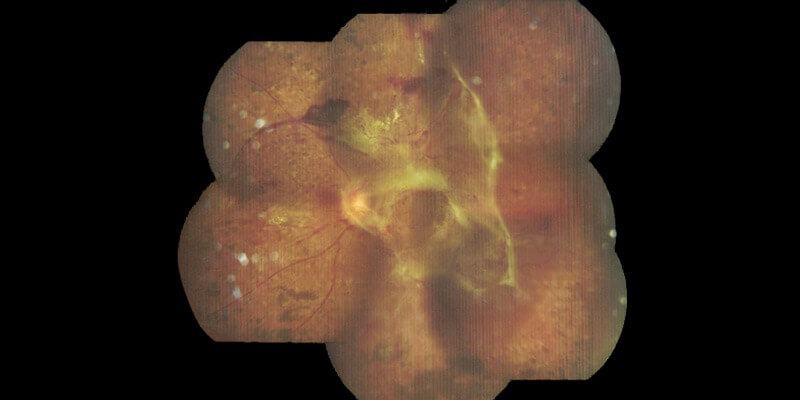
Diabetic retinopathy is a serious eye condition that affects people with diabetes, both Type 1 and Type 2. It occurs when high blood sugar levels cause damage to the blood vessels in the retina, the part of your eye responsible for vision. This damage can lead to vision loss if left untreated. The condition is often linked to the duration of diabetes and poor blood sugar control, making it essential for individuals with diabetes to monitor their eye health regularly.
In the early diabetic retinopathy stages, it may not present obvious symptoms. However, over time, it can progress and lead to complications that affect your vision.
What Are the Symptoms of Diabetic Retinopathy?
In its early diabetic retinopathy stages, it might not cause any noticeable symptoms. That is why regular eye exams are crucial for those with diabetes. As the condition worsens, the following symptoms may appear:
- Blurry or diminished vision
- The appearance of floaters or black spots in your vision
- Dark areas in the visual field
- Possible complete vision loss in severe cases
What Causes Diabetic Retinopathy?
Diabetic retinopathy occurs when high blood sugar levels damage the blood vessels in the retina. These vessels may leak fluid or become blocked, affecting the retina’s ability to receive proper nourishment. The main risk factors include:
- Poor blood sugar control
- Long duration of diabetes
- Pregnancy
- High blood pressure (hypertension)
- High cholesterol (hypercholesterolemia)
- Smoking
How Is Diabetic Retinopathy Diagnosed?
A comprehensive eye examination is the best way to diagnose this condition. The tests may include:
- Visual Acuity Testing: Measures how well you can see at different distances.
- Tonometry: Assesses the pressure inside your eye.
- Pupil Dilation: Eye drops are used to widen the pupil, allowing the doctor to inspect the retina and optic nerve.
- Optical Coherence Tomography (OCT): Provides detailed images of the retina using light waves.
- Fluorescein Angiography: Used to detect leaky or damaged blood vessels, often in advanced diabetic retinopathy stages
What Are the Diabetic Retinopathy Stages?
Diabetic retinopathy is typically divided into four stages, each representing the severity of the condition:
- Mild Nonproliferative Retinopathy: The earliest stage, where small blood vessels in the retina swell.
- Moderate Nonproliferative Retinopathy: More blood vessels become blocked, affecting blood flow to the retina.
- Severe Nonproliferative Retinopathy: Many blood vessels are blocked, causing serious damage to the retina.
- Proliferative Diabetic Retinopathy: The most advanced stage, where new, abnormal blood vessels begin to form and can lead to bleeding and retinal detachment.
The earlier the stage, the better the prognosis with proper diabetic retinopathy treatment. Catching it early is key to preventing permanent damage.
What Are the Treatment Options for Diabetic Retinopathy?
Treatment for this condition depends on the severity of the condition. Early intervention can prevent further vision loss, so it is vital to seek medical help if you experience any symptoms.
- Diabetic Retinopathy Treatment for Early Stages: In the early diabetic retinopathy stages, controlling your blood sugar levels and managing other risk factors (like blood pressure and cholesterol) is crucial. This can help slow the progression of the disease.
- Laser Treatment: As the condition progresses, laser treatment may be necessary. This treatment targets areas of the retina with damaged blood vessels to prevent further leakage or bleeding. While it does not improve vision, it can stop further vision loss.
- Injections for Macular Oedema: If fluid accumulates in the macula (the central part of the retina responsible for sharp vision), injections may be used to reduce swelling and improve vision.
- Vitrectomy: In severe cases, where laser treatment is not effective, a vitrectomy may be performed. This surgery involves removing the vitreous gel from the eye and replacing it with a clear solution. Scar tissue and blood may also be removed to prevent further damage.
What Are the Risks of Diabetic Retinopathy?
If left untreated, this condition can lead to several serious eye problems:
- Vision loss: Can occur due to swelling, bleeding, or retinal detachment.
- Glaucoma: Increased pressure within the eye, which can damage the optic nerve.
- Blindness: In severe cases, this condition can lead to complete blindness, making regular eye exams and treatment crucial.
How Can You Prevent Diabetic Retinopathy?
The most important way to prevent or slow the progression of diabetic retinopathy is by controlling your blood sugar levels. Additional steps include:
- Maintaining healthy blood pressure and cholesterol levels
- Avoiding smoking
- Regular eye check-ups with an ophthalmologist
After undergoing diabetic retinopathy treatment, it is also advisable to avoid heavy lifting and strenuous physical activity for a short period to allow for recovery and reduce the risk of further damage.
How Can Neoretina Eyecare Institute Help?
At Neoretina Eyecare Institute, we understand how challenging living with diabetes can be, especially when it comes to managing eye health. With advanced diagnostic tools and a team of experienced specialists, we offer tailored treatment plans for diabetic retinopathy to preserve your vision. Early detection and treatment are key, and we are here to guide you every step of the way. Trust our experts to provide compassionate, cutting-edge care for all your diabetic retinopathy treatment needs.
FAQ’s
In the early diabetic retinopathy stages, symptoms may not be noticeable. However, blurred vision, floaters, or dark areas in your visual field may develop over time. Regular eye exams are crucial for early detection and diabetic retinopathy treatment.
Diabetic retinopathy treatment varies depending on the stage. Early stages may only require blood sugar control, while later stages may need laser treatment, injections, or vitrectomy. Timely intervention is key to preventing vision loss.
Yes, if left untreated, diabetic retinopathy can lead to blindness due to retinal damage, glaucoma, or retinal detachment. Early diagnosis and appropriate diabetic retinopathy treatment can help prevent permanent damage and preserve vision.
- High Blood Pressure and Vision: How Your Eyes Show the Warning Signs - May 27, 2026
- Can the 20-20-20 Rule Protect Your Eyes from Digital Strain? - May 27, 2026
- Can Swimming Cause Eye Infections? Summer Eye Safety Tips - April 27, 2026